Hair Loss Injections: What the Evidence Actually Says
Australian clinics offer hair loss injections with considerable confidence. The clinical evidence tells a more careful story. This article does something most clinic brochures don't it looks honestly at what the research actually shows, what remains genuinely unresolved, and what that means for anyone deciding whether to invest in a course of treatment.
What Are Growth Factor Hair Loss Injections?
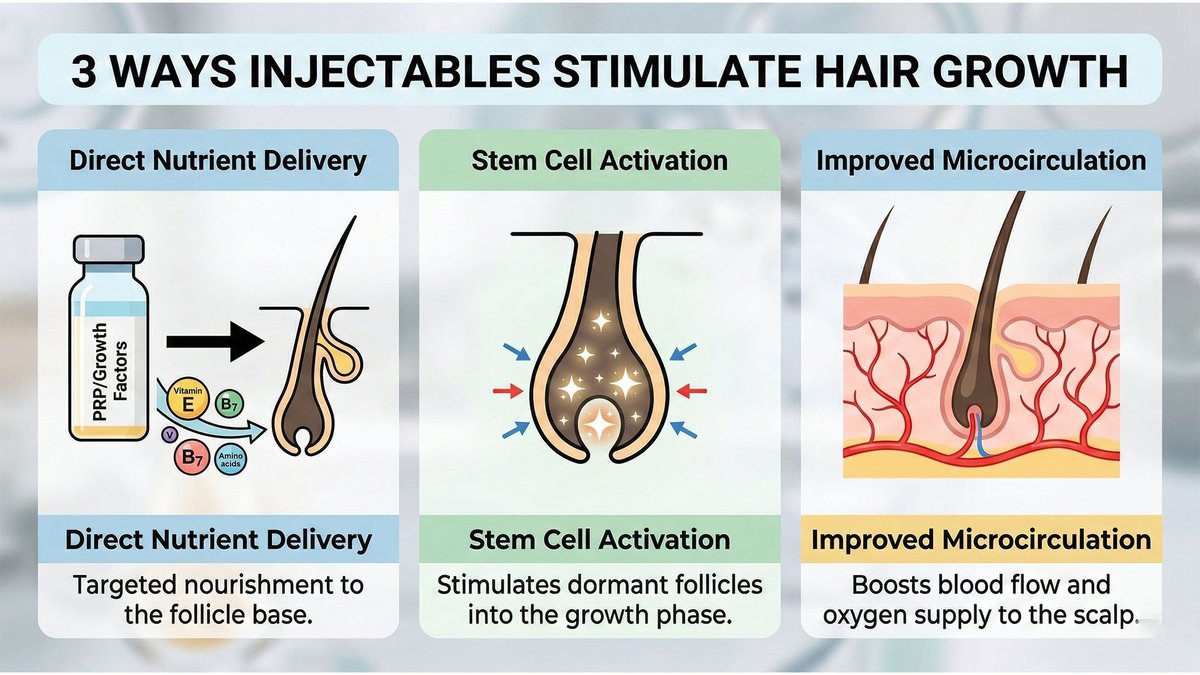
The two most common forms of growth factor injection used in hair loss clinics are PRP (Platelet-Rich Plasma) and PRF (Platelet-Rich Fibrin). Both are autologous treatments, meaning they are derived from the patient's own blood, and both are built around the same underlying biological rationale: that concentrating and reinjecting growth factors into the scalp may support the follicular environment and slow the progression of hair thinning.
In both cases, a small volume of blood is drawn, placed into a centrifuge, and processed to isolate a fraction concentrated in platelets. Those platelets release growth factors including PDGF, VEGF, FGF, IGF-1, and TGF-beta that may theoretically signal hair follicle stem cells. In laboratory settings, these signals are measurable and the cellular activity is well documented. The meaningful distinction between PRP and PRF lies in how each is prepared, what that preparation produces biologically, and whether one holds a clinical advantage over the other in real patients. That comparison is explored in full in the companion article linked above. What this article addresses is the harder and more immediately useful question: regardless of which variant a clinic is offering, what does the clinical evidence actually support?
What Does the Clinical Evidence Actually Show?
This is where an honest account has to diverge from most of what is published in clinic marketing materials.
The peer-reviewed evidence for both PRP and PRF in hair loss is limited and inconsistent. A systematic review by Greco et al., published in Dermatologic Surgery in 2021, concluded that while results have been described as promising in some smaller studies, the body of evidence remains insufficient to support confident clinical recommendations for either treatment. An earlier meta-analysis by Sclafani and Sclafani, published in Facial Plastic Surgery Clinics of North America in 2013, reached broadly similar conclusions about the quality and consistency of the available data.
The methodological problems in the existing literature are significant. Most human trials involve between 20 and 50 participants, which is far too small a sample to draw generalisable conclusions. Many studies lack proper control groups or blinding, meaning it is difficult to separate genuine treatment effects from placebo responses. Reported outcomes vary considerably across studies: some suggest modest improvements in hair density and follicle diameter, while others show no meaningful difference compared to saline injections. And critically, no randomised controlled trial has directly compared PRP against PRF in a head-to-head study for hair loss. The widespread clinical claim that PRF is categorically superior to PRP is, at present, not supported by comparative trial data.
The cellular mechanism is theoretically sound. The human clinical evidence, as it currently stands, simply has not caught up.
 ---
---
The Standardisation Problem
One of the most underappreciated issues in this field is that there is no agreed-upon protocol for either treatment, and this makes comparing studies, and evaluating clinic offerings, almost impossible.
Two clinics both advertising PRP may be using entirely different preparations. Across published studies, researchers have used centrifugation speeds ranging from 1,000 to 3,500 RPM, platelet concentrations anywhere from 150,000 to over one million platelets per microlitre, injection frequencies ranging from monthly to quarterly, and treatment courses of anywhere between three and six or more sessions. Greco et al. explicitly identified this lack of standardisation as the primary reason the evidence remains inconclusive. Until agreed protocols are established and consistently applied across clinical settings, the "PRP works" or "PRF works" headline is, at best, an incomplete sentence.
This matters for consumers and for clinicians alike. A patient who does not respond to one clinic's PRP protocol cannot assume that PRP as a treatment category has failed for them. They may simply have received a protocol that delivered a different platelet concentration, or a different injection frequency, to the study they read about. The variance is that significant.


 ---
--- ---
---